IVF Options After Age of 40 and 50: What You Need to Know
What if the dream of parenthood doesn’t fade with time? For many, the idea of starting a family later in life feels like navigating uncharted territory, but modern medicine continues to redefine possibilities. While fertility naturally declines with age, advancements in reproductive care offer pathways that were once unimaginable. IVF Options After age of 40 and 50 years remain one of the most important topics for both intended parents and fertility experts.
Age remains a critical factor in fertility, yet it doesn’t have to be a barrier. This article explores how medical innovations address challenges like diminished egg quality and hormonal changes. Whether using one’s own eggs or donor materials, personalized strategies can improve outcomes.
Key Takeaways
- Fertility declines with age, but modern treatments expand opportunities for conception.
- Using donor eggs often improves success rates compared to using one’s own eggs later in life.
- Pregnancy outcomes depend on individual health factors, not just chronological age.
- Medical teams now create customized plans to address hormonal and biological challenges.
- Emotional support is a critical component of the journey for older patients.
📞 Get in Touch for a Free Surrogacy Consultation
📱 +91-8800481100 (WhatsApp | LINE | Viber)
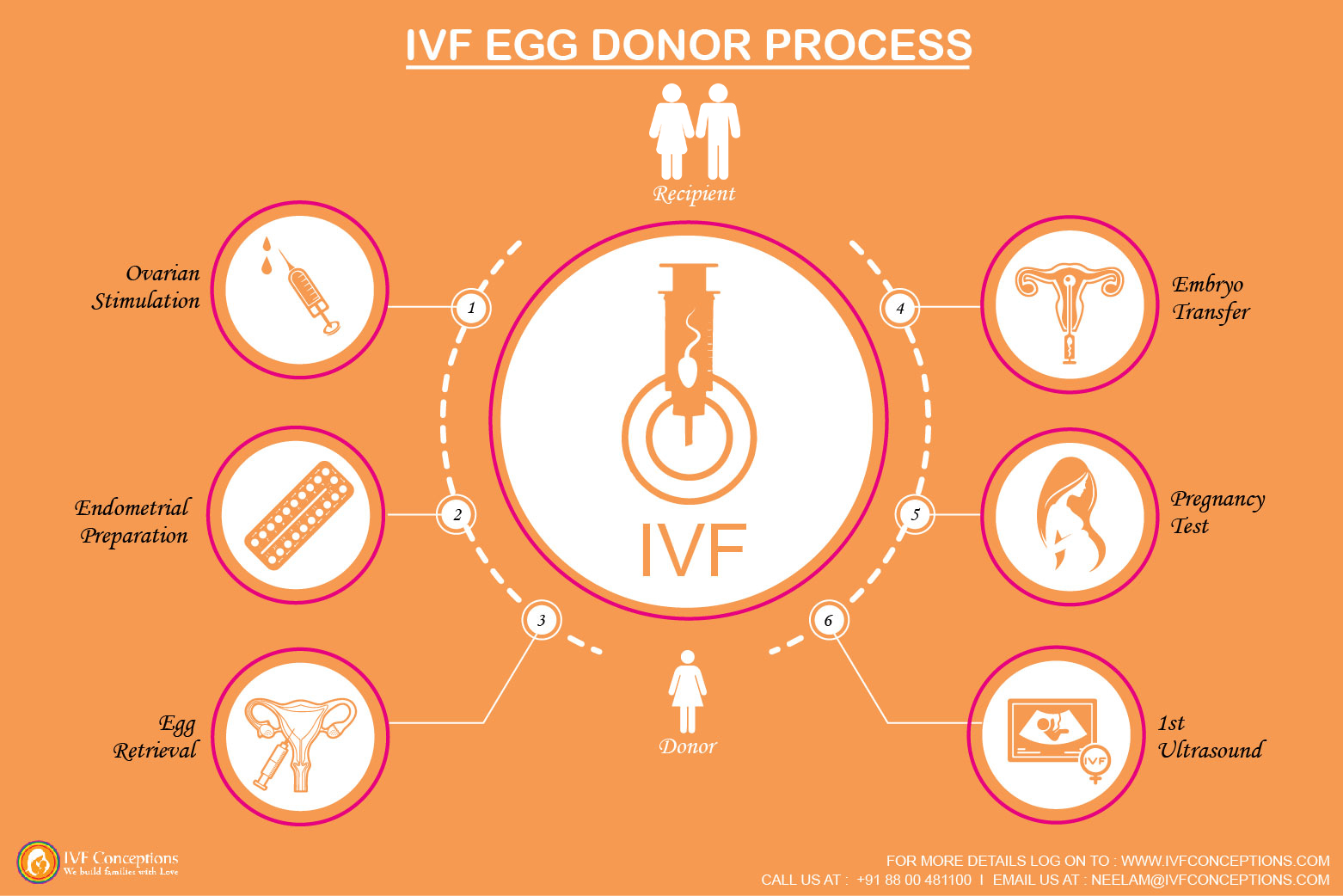
Introduction: Is IVF Still an Option After 40 or 50?
Fertility changes with age, but parenthood is still possible for many women in their 40s and even 50s thanks to advancements in In Vitro Fertilization (IVF).
While age naturally lowers egg quality and quantity, modern IVF techniques — including donor eggs, embryo freezing, and hormonal therapies — have opened doors for hopeful parents well beyond their reproductive peak.
How Age Affects Female Fertility
| Age Range | Natural Conception Chance per Cycle | Common Fertility Issues |
| 20–30 | 20–25% | Minimal |
| 35–39 | 10–15% | Declining egg quality |
| 40–44 | 5–10% | Low AMH, increased miscarriage risk |
| 45+ | <1–2% | Menopause, egg depletion |
Key Takeaway: Egg quantity and quality decline sharply after 35, especially after 40. IVF with your own eggs becomes less viable with age, but donor egg IVF offers high success rates.
IVF After 40: What Are Your Options?
1. IVF with Own Eggs (40–44)
- Still possible in the early 40s, but with reduced success rates.
- May require multiple cycles.
- Preimplantation Genetic Testing (PGT-A) is recommended to select chromosomally normal embryos.
Success Rate (Own Eggs at 40–42): ~15–20% per cycle Success Rate (Own Eggs at 43–44): <5–10% per cycle
2. IVF with Donor Eggs
- The most recommended option for women over 43.
- Donor eggs from women aged 21–30 offer higher success and lower miscarriage risk.
Success Rate (Donor Eggs, Any Age): ~50–60% per cycle ✅ Best option for those with low AMH or poor ovarian reserve.
3. Embryo Adoption
- Use frozen embryos from other couples who completed IVF.
- Lower cost than donor egg IVF.

IVF Options After age of 40 and 50
IVF After 50: Is It Still Possible?
Yes — but mostly using donor eggs and with strong medical screening. IVF clinics will assess:
- General health & uterine receptivity
- Cardiovascular risk
- Hormonal preparation for embryo transfer
Women over 50 are typically prescribed Hormone Replacement Therapy (HRT) to prepare the uterus for pregnancy.
Comparison Table: IVF Options After 40 & 50
| Option | Best Age Group | Success Rate | Key Considerations |
| IVF with Own Eggs | 40–42 | 10–20% | Depends on ovarian reserve & egg quality |
| IVF with Donor Eggs | 43+ | 50–60% | Higher cost, legal/ethical aspects vary |
| Embryo Adoption | 45–50+ | ~45% | Budget-friendly, limited embryo choices |
| IVF with Partner’s Sperm | 40–50+ | Depends on egg source | Ensure sperm testing and DNA integrity |
Understanding Fertility Challenges in Advanced Maternal Age
Biological clocks may tick louder with age, yet modern insights offer clarity on conception barriers. For women over 35, reproductive health shifts in ways that require careful navigation. The primary concern? A natural decline in ovarian reserve, which reduces both egg quantity and quality over time.
Ovarian reserve peaks in a person’s 20s and drops sharply after 35. By 40, many individuals have fewer than 10% of their original egg supply. This decline impacts not just numbers but also genetic integrity—older eggs face higher risks of chromosomal abnormalities.

Hormonal changes further complicate conception. Estrogen and progesterone levels fluctuate, affecting ovulation regularity. Additionally, age-related health factors like blood pressure or insulin resistance can influence fertility outcomes. It’s not just about biology—lifestyle and preexisting conditions also play roles.
| Factor | Impact | Role of Health |
| Ovarian Reserve | Reduces egg quantity | Cannot be reversed |
| Hormonal Changes | Affects ovulation cycles | Managed through therapy |
| Overall Health | Influences implantation | Improved via lifestyle |
Clinicians emphasize that maternal age and health jointly shape success rates. While time affects ovarian reserves, proactive care—like monitoring vitamin levels or thyroid function—can optimize outcomes. Later sections will explore diagnostic tests to assess these factors.
Understanding these challenges helps patients make informed choices. Knowledge empowers individuals to collaborate with specialists, blending science with personalized strategies.
The Impact of Age on Fertility
Age reshapes fertility in ways that demand both awareness and adaptation. Two interconnected factors—ovarian reserve and genetic integrity—play pivotal roles in conception potential. While these challenges are natural, understanding them helps in making informed decisions.
Egg Quantity and Ovarian Reserve
Women are born with a finite number of eggs, which decreases significantly after 35. By 40, most have less than 10% of their original ovarian reserve. This reduction impacts treatment plans, as fewer available eggs mean fewer opportunities for viable embryos.
- Ovarian reserve tests measure the remaining egg supply via hormone levels and ultrasound.
- Lower reserves often require adjusted medication protocols during stimulation cycles.
Decline in Egg Quality and Genetic Factors
Quality matters as much as quantity. Older eggs are more likely to develop chromosomal errors, increasing miscarriage risks. One study found that over 50% of eggs from women aged 40+ show genetic abnormalities.
Preimplantation genetic testing (PGT-A) screens embryos for these issues, improving selection accuracy. Clinics frequently recommend this step to prioritize healthier embryos for transfer.
“Genetic screening doesn’t guarantee success, but it significantly refines the process,” notes a 2023 reproductive endocrinology review.
| Age | Average Eggs Remaining | Normal Embryo Rate |
| 35 | ~25,000 | 40% |
| 40 | ~5,000 | 15% |
| 45 | ~1,000 | 5% |
Proactive steps like lifestyle adjustments or early testing can’t reverse time—but they help optimize existing resources. Collaboration with specialists ensures strategies align with biological realities.
IVF options after 40 and 50
Modern reproductive care offers multiple approaches for those exploring pregnancy in their 40s and 50s. Clinics design personalized protocols based on individual health markers, ovarian function, and genetic factors. This customization helps address unique biological challenges while maximizing potential success.
Two primary pathways exist: using one’s own eggs or donor materials. While conventional methods with personal eggs remain an option, many women benefit from adjusted stimulation protocols to improve egg retrieval numbers. For example, lower-dose medications or dual stimulation cycles may enhance outcomes.
Donor eggs often become a practical choice when ovarian reserves are critically low. These treatments IVF specialists recommend typically involve thorough donor screening and synchronized hormone cycles. Success rates with donor materials are notably higher, offering renewed optimism.
| Approach | Key Features | Considerations |
| Own Eggs | Genetic connection | Lower embryo viability |
| Donor Eggs | Higher success rates | Emotional adjustment |
Emerging technologies like time-lapse embryo monitoring or mitochondrial augmentation also show promise. While not guaranteed, these innovations refine selection processes and support healthier embryo development.
“Every patient’s journey is distinct—our role is to match science with their specific circumstances,” explains a leading fertility specialist.
Open communication with medical teams ensures alignment between expectations and biological realities. This collaborative approach empowers individuals to navigate choices confidently.
Exploring Success Rates and Treatment Challenges
Understanding treatment outcomes requires navigating both optimism and biological realities. Age significantly influences conception probabilities, but data-driven insights help clarify expectations. This section examines how success rates shift with different approaches and what challenges may arise.
Comparing Success with Own Eggs and Donor Eggs
Pregnancy chances decline sharply as ovarian reserves diminish. For women over 40, success rates using personal eggs drop below 15% per cycle, according to CDC data. Donor materials, however, maintain rates above 50% regardless of maternal age.
| Age Group | Own Eggs Success | Donor Eggs Success |
| Under 35 | 55% | 55% |
| 35-37 | 40% | 50% |
| 38-40 | 25% | 50% |
| 41-42 | 12% | 45% |
| 43-44 | 3% | 40% |
Key factors behind this gap include:
- Higher rates of chromosomal abnormalities in older eggs
- Reduced response to fertility medications
- Increased miscarriage risks after conception
Statistical Insights and Medical Studies
A 2022 study found that women over 42 using donor eggs had three times higher live birth rates than those using personal eggs. However, pregnancy complications like gestational diabetes remain more common in older recipients.
“While donor materials improve outcomes, thorough health screenings are essential for all parties,” states a recent JAMA fertility analysis.
These statistics highlight why clinics emphasize personalized risk assessments. The next section explores diagnostic tools that help tailor treatment plans to individual needs.
Assessing Ovarian Reserve and Egg Quality
Accurate diagnostics lay the foundation for informed fertility journeys. Specialists use advanced tools to evaluate biological potential, ensuring treatment plans align with individual realities. These assessments clarify what steps may improve the chance of getting pregnant while managing expectations.
IVF Options After age of 40 and 50
Key Evaluations for Personalized Care
Three primary tests gauge ovarian health:
- AMH blood tests measure anti-Müllerian hormone levels, indicating the remaining egg supply.
- Antral follicle count ultrasounds visualize developing follicles, reflecting monthly egg recruitment.
- FSH testing tracks follicle-stimulating hormone spikes, signaling declining reserve.
Results help clinics predict how many viable eggs might respond to stimulation. This data directly influences medication dosages and embryo transfer timing. For example, low AMH often prompts earlier retrieval cycles to capture healthier eggs.
| Test | Purpose | Role in Planning |
| AMH | Assess egg quantity | Determine stimulation protocol |
| Ultrasound | Count active follicles | Predict retrieval numbers |
| FSH | Evaluate hormonal balance | Adjust cycle start dates |
Advantages and Risks of IVF in Later Years
Pursuing conception later in life involves balancing hope with medical realities. While advanced maternal age introduces unique challenges, modern protocols aim to mitigate risks while prioritizing safety. Understanding both possibilities and precautions helps individuals make empowered choices.
Potential Health and Pregnancy Risks
Women over 40 face higher rates of complications during fertility treatments. Conditions like gestational diabetes occur 2-3 times more frequently compared to younger age groups. Elevated blood pressure and preeclampsia risks also rise, particularly after 45.
| Risk Factor | Under 35 | 35-40 | 40+ |
| Gestational Diabetes | 3% | 7% | 15% |
| High Blood Pressure | 4% | 9% | 18% |
| Preterm Birth | 8% | 12% | 22% |
Despite these statistics, many achieve a healthy pregnancy through careful monitoring. The American College of Obstetricians recommends:
- Preconception cardiovascular screenings
- Early glucose tolerance tests
- Frequent prenatal checkups
“Age alone doesn’t disqualify someone from success—it simply requires tailored care plans,” states a 2023 ACOG guideline.
Clinics now use predictive analytics to personalize treatment schedules. This approach reduces strain on the body while optimizing embryo viability. For those at higher pregnancy age-related risks, specialists often suggest single embryo transfers to lower complication chances.
Stories of healthy pregnancy outcomes remind us that risks don’t equal certainties. With proper medical support, many navigate this journey successfully. Next, we’ll explore how clinical guidelines shape these strategies.
Treatment Considerations and Clinical Guidelines

IVF Options After age of 40 and 50
Medical teams prioritize patient-specific factors to craft treatment pathways that balance hope with evidence. Personalized protocols begin with evaluating ovarian function, hormone levels, and preexisting conditions like diabetes or hypertension. These assessments ensure therapies align with biological realities while minimizing risks.
Clinical guidelines from organizations like the American Society for Reproductive Medicine emphasize safety through:
- Comprehensive cardiac and metabolic screenings
- Individualized medication dosing based on response patterns
- Regular monitoring of treatment progress
| Factor | Clinical Impact | Guideline Reference |
| BMI | Affects medication absorption | ASRM 2022 |
| AMH Levels | Guides stimulation protocols | SART 2023 |
| Thyroid Function | Influences implantation success | ACOG 2021 |
Treatment plans are not one-size-fits-all. For example, women with diminished ovarian reserve may receive lower-dose stimulants to reduce hyperstimulation risks. Clinics also weigh emotional readiness, as stress impacts cycle outcomes.
“Adherence to guidelines protects patients while maintaining realistic success benchmarks,” states a recent ASRM committee report.
Informed individuals benefit from clinics that transparently explain success probabilities and potential complications. This collaborative approach fosters trust, ensuring decisions reflect both medical expertise and personal values.
IVF with Own Eggs: Possibilities and Limitations
Exploring conception with one’s own genetic material requires balancing hope with biological realities. While advancements offer pathways, age-related factors heavily influence outcomes. Success hinges on two critical elements: the quantity of viable embryos and their genetic health.
Donor Egg IVF: A Popular Route After 43+
Benefits:
- High success rate
- Lower risk of genetic abnormalities
- Shorter time to pregnancy
How It Works:
- Select an egg donor (anonymous or known)
- Donor undergoes stimulation and egg retrieval
- Fertilization with partner’s or donor sperm
- Embryo transfer into the intended mother’s uterus
Realistic Expectations for Success
Women using their own eggs face declining success rates as ovarian reserves diminish. After 40, chromosomal abnormalities in embryos rise sharply—studies show over half may have genetic errors. This reduces the likelihood of healthy implantation and increases miscarriage risks.
Clinics often recommend preimplantation genetic testing (PGT) to identify embryos with the best potential. However, even with screening, live birth rates remain below 15% per cycle for those over 42. Factors like hormonal balance and follicle response further impact results.
| Age | Average Viable Embryos | Live Birth Rate |
| Under 35 | 4-6 | 40% |
| 40-42 | 1-2 | 12% |
| 43+ | 0-1 | <5% |
Specialized clinics tailor protocols to maximize egg retrieval and embryo quality. Dual stimulation cycles or personalized medication dosages may improve outcomes. It’s essential to choose a clinic with expertise in treating older patients, as nuanced care can make a meaningful difference.
“Individualized approaches are non-negotiable when working with diminished ovarian reserves,” emphasizes a 2023 report from the Society for Assisted Reproductive Technology.
While success with personal eggs becomes rare after 45, exceptions exist. Thorough testing and realistic goal-setting ensure emotional and physical preparedness for the journey ahead.

IVF Options After the age of 40 and 50
Utilizing Donor Eggs for Enhanced Outcomes
Choosing donor materials can redefine possibilities for those facing biological hurdles. When ovarian reserves decline, using donor eggs often becomes the most viable path to conception. Clinics worldwide report success rates exceeding 50% with this approach—a stark contrast to single-digit percentages when relying on personal eggs after 40.
Rigorous Screening for Optimal Results
Reputable programs implement multi-step evaluations to ensure donor health and genetic integrity. Candidates undergo:
- Comprehensive medical history reviews
- Genetic carrier screening for 200+ conditions
- Psychological assessments and infectious disease testing
This process minimizes risks while matching recipients with profiles aligning with their preferences. One California clinic notes that 98% of donors pass initial screenings, but only 30% meet final approval criteria.
| Age Group | Own Eggs Success | Donor Eggs Success |
| Over 40 | 4-12% | 52-60% |
| Over 45 | <3% | 48-55% |
Leading centers like Cyprus IVF Hospital and New York Fertility Institute showcase how specialized donor egg IVF programs achieve consistent results. Their protocols synchronize recipient cycles with donor retrievals, optimizing hormonal timing.
“Donor materials bridge biological gaps while maintaining rigorous health standards—this dual focus transforms outcomes,” explains a Greek clinic’s medical director.
With advanced screening and tailored protocols, using donor eggs offers realistic pathways to healthy pregnancies where other methods falter. This approach balances science with compassionate care, honoring the dream of parenthood.
Choosing the Right Clinic
Look for IVF clinics that:
- Specialize in older women or donor IVF
- Have transparent success rates
- Offer personalized hormonal protocols
- Provide genetic counseling and PGT-A testing
👉 Tip: Consider international clinics (e.g., in Georgia, Ukraine, Greece, or Mexico) for more affordable donor egg IVF options.
IVF Treatment Cost
Navigating the financial landscape of fertility treatments requires both clarity and strategic planning. Expenses vary widely based on location, clinic reputation, and required procedures. For example, rates IVF specialists charge in the U.S. often range from $12,000 to $25,000 per cycle—excluding medications or genetic testing.
International options may reduce costs. Clinics in Europe or Asia sometimes offer comparable services at 30-50% lower prices. However, travel logistics and follow-up care add hidden expenses. Treatment packages often bundle services like monitoring or embryo storage, providing predictable budgeting.
| Clinic Location | Average Cost | Notes |
| United States | $15,000-$30,000 | Excludes medications |
| Europe | $7,000-$12,000 | Includes basic testing |
| Asia | $5,000-$10,000 | Limited insurance options |
Many IVF programs now provide refund guarantees for multiple cycles. These plans cost more upfront but protect against repeated financial losses. Patients should ask:
- What diagnostic tests are included?
- Are donor material fees separate?
- Does insurance cover genetic screenings?
“Understanding payment structures prevents surprises—always request itemized estimates,” advises a New York fertility financial counselor.
Evaluating loans, grants, or clinic financing helps manage expenses. While rates IVF clinics advertise matter, holistic planning ensures families pursue parenthood without unsustainable debt.

Personalized Treatment Protocols for Older Women
Tailored care plans are revolutionizing fertility journeys for women in their later reproductive years. Clinics now prioritize hormone optimization and cycle adjustments to address age-related biological shifts. This approach balances scientific precision with emotional well-being, creating pathways that respect individual needs.
Adapting Hormone Therapies for Precision
Older women often require modified medication protocols to maximize ovarian response. Lower-dose stimulants like mini-IVF reduce physical strain while targeting healthier follicles. Clinicians also adjust estrogen priming or progesterone support based on hormone panels and prior cycle data.
Stimulation Strategies for Quality Over Quantity
Egg quality becomes paramount when reserves diminish. Dual stimulation cycles—retrieving eggs in two phases of the menstrual cycle—help capture more viable candidates. Time-lapse embryo monitoring further refines selection, prioritizing those with optimal development patterns.
| Protocol | Purpose | Outcome |
| Mini-IVF | Gentle stimulation | Reduces side effects |
| Dual Stimulation | Double retrieval | Increases viable eggs |
| PGT-A Screening | Genetic analysis | Lowers miscarriage risk |
Integrating counseling into treatment plans addresses the unique emotional challenges older women face. Many clinics offer sessions with therapists specializing in fertility journeys, helping patients navigate complex decisions like donor material use.
“Personalization isn’t just medical—it’s about honoring each patient’s physical and emotional landscape,” explains Dr. Emily Torres of San Diego Fertility Center.
These protocols reflect modern fertility care’s evolution: data-driven yet deeply human. By aligning science with individual circumstances, clinics empower older women to pursue parenthood with clarity and confidence.
Medical Screening Before IVF After 40 or 50
Before starting IVF, clinics may require:
- Hormonal blood tests (AMH, FSH, LH)
- Antral follicle count via ultrasound
- Pap smear, mammogram (esp. after 45)
- ECG and cardiac risk assessment
These ensure the safety of carrying a pregnancy at a later age.
Lifestyle Modifications to Boost IVF Success
Small daily choices can create ripples of change in fertility journeys. Research shows targeted lifestyle adjustments may improve outcomes by supporting hormonal balance and cellular health. These strategies work alongside medical treatments, creating a foundation for better results.
Nutrition plays a pivotal role. Mediterranean-style diets rich in antioxidants and omega-3s correlate with higher embryo quality. Key supplements include:
- CoQ10: May enhance egg mitochondrial function
- Vitamin D: Supports hormone regulation
- Prenatal vitamins: Ensure folate levels for fetal development
Regular physical activity improves blood flow to reproductive organs. Aim for 150 minutes weekly of moderate exercise like swimming or brisk walking. Maintaining a healthy BMI (18.5-24.9) helps regulate estrogen production and insulin sensitivity.
| Stress Reduction Method | Frequency | Benefit |
| Mindfulness meditation | Daily 10-minute sessions | Lowers cortisol levels |
| Yoga | 3x weekly | Improves pelvic circulation |
| 7-9 hours sleep | Nightly | Balances reproductive hormones |
A 2022 Harvard study found women practicing stress-reduction techniques had 20% higher implantation rates. “Mental well-being directly impacts physiological processes,” notes lead researcher Dr. Alicia Chen.
Holistic approaches blend these elements into sustainable routines. Patients report feeling empowered when actively contributing to their care plans. While not replacements for medical interventions, these modifications create environments where treatments can thrive.
Conclusion for IVF Options After age of 40 and 50
Thanks to scientific advances in reproductive medicine, age is no longer a full stop on the road to parenthood. While challenges increase with age, options like donor egg IVF and embryo adoption offer real, successful paths to pregnancy after 40 and even 50.
The path to parenthood later in life blends science with deeply personal choices. While biological hurdles exist, modern fertility treatments offer tailored strategies to navigate them. Education empowers patients to collaborate with specialists, turning challenges into actionable plans.
Key discussions highlighted how ovarian health, genetic screening, and clinic selection shape outcomes. Personalized protocols—from hormone adjustments to donor materials—prioritize safety while optimizing success. Emotional resilience remains vital, as does partnering with accredited teams who align care with individual needs.
📞 Get in Touch for a Free Surrogacy Consultation
📱 +91-8800481100 (WhatsApp | LINE | Viber)
💫 Why Intended Parents Choose Complete Surrogacy for a Safe, Smooth & Successful Surrogacy Journey:
🌍 Access to multiple surrogacy destinations with 15+ years of international experience
🏥 Partnerships with top-tier fertility clinics and agencies, backed by references from past clients
👩🦱 Diverse egg donor options: Asian, Caucasian, African, Oriental, and more
💸 Transparent and affordable pricing—direct payments with no extra agency fees
🔒 No hidden costs—all charges are agreed upon upfront
🤝 Dedicated case manager for personalized support
📲 Fast, honest, and clear communication throughout
📑 Full legal support for visas, documentation, and baby exit processes
🚚 Assistance with frozen sperm/embryo shipment logistics
FAQ for IVF Options After 40 and 50:
Can women over 40 achieve pregnancy with their own eggs through IVF?
While possible, success rates decline significantly after 40 due to reduced ovarian reserve and egg quality. Most clinics recommend genetic testing of embryos or considering donor eggs to improve the chances of a healthy pregnancy.
How do donor eggs improve outcomes for older women?
Donor eggs from younger individuals typically have higher genetic quality, leading to better embryo development and pregnancy rates. Studies show donor egg IVF success rates remain stable regardless of the recipient’s age.
What health risks should older patients consider before treatment?
Advanced maternal age increases the risks of gestational diabetes, hypertension, and chromosomal abnormalities. Clinics perform thorough health screenings and may recommend single embryo transfer to reduce complications.
Are there financial assistance programs for multiple IVF cycles?
Many clinics offer bundled packages or refund programs for multiple cycles. Insurance coverage varies, but some states mandate partial fertility treatment coverage—always verify policies during clinic consultations.
What criteria matter most when choosing a fertility clinic?
Look for clinics with high live birth rates for your age group, transparent data reporting, and expertise in personalized protocols. Accreditation by organizations like SART ensures adherence to quality standards.
Does preimplantation genetic testing benefit older patients?
Yes. PGT-A screens embryos for chromosomal abnormalities, reducing miscarriage risks and improving implantation rates. This is particularly valuable when using your own eggs with age-related quality concerns.
Can lifestyle changes enhance IVF success in later years?
Optimizing BMI, managing stress, and avoiding toxins like nicotine may improve outcomes. However, these adjustments can’t reverse age-related egg depletion—realistic expectations are crucial.
Is there an age cutoff for donor egg IVF in the U.S.?
Most clinics set limits between 50-55 due to pregnancy health risks. Exceptions require thorough cardiac and obstetric evaluations to ensure patient safety during treatment and delivery.
Additional guides:

